Diabetic Foot Complications: Treatment & Prevention in Whitby
Diabetes can lead to serious foot complications, including ulcers, infections, and slow‑healing wounds. Reduced sensation and poor circulation mean that even a small blister or cut can progress quickly. Early assessment and ongoing foot care significantly reduce the risk of infection and amputation. We provide diabetic foot treatment, monitoring, and preventative care at our Whitby clinic to help protect long‑term mobility.
Why Diabetic Foot Complications Develop
Diabetes affects the feet in two major ways:
-
Neuropathy reduces sensation, making it difficult to feel cuts, pressure, or injury.
-
Poor circulation slows healing and increases the risk of infection.
When these occur together, a minor wound can become a medical emergency. Many diabetic ulcers begin as unnoticed blisters, calluses, or pressure points.
Common Diabetic Foot Complications
Ulcers and Wounds
Foot ulcers often develop from friction, pressure, or unnoticed injuries. Without proper care, they can become infected and lead to tissue damage.
- Neuropathy prevents early detection.
- Poor blood flow delays healing.
- Infection can spread quickly if untreated.
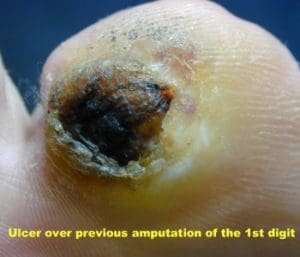
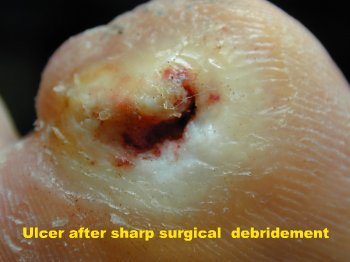
The ulcer case below shows how sharp debridement and pressure offloading can support healing. the occurred over 6 weeks
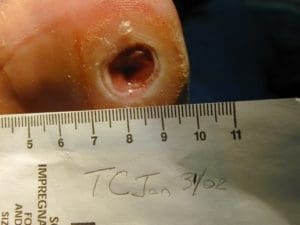
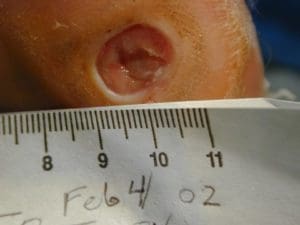
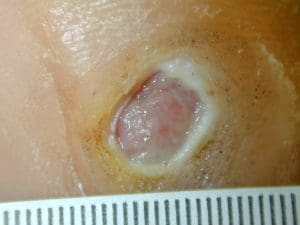
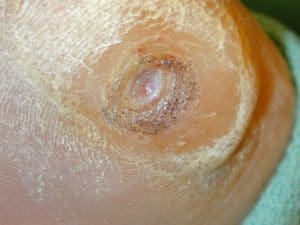
Infections
Infections can develop rapidly in diabetic feet. Redness, warmth, swelling, or drainage require immediate attention. Untreated infections can spread to deeper tissues or bone.
Amputations
Up to 80% of lower‑limb amputations are linked to diabetes. Most amputations begin with a preventable ulcer. Early care, proper footwear, and routine monitoring dramatically reduce this risk.

How We Assess Diabetic Foot Complications
A diabetic foot assessment includes:
-
Sensation testing (neuropathy screening)
-
Circulation evaluation
-
Skin and nail examination
-
Identification of pressure points
-
Footwear assessment
-
Wound evaluation (if present)
This allows us to determine the severity of the complication and the safest treatment plan.
Treatment Options for Diabetic Foot Complications
Wound Care & Debridement
Removal of dead or infected tissue helps wounds heal more effectively and reduces infection risk. Your current page shows a wound healed over six weeks using sharp debridement and pressure offloading.
Offloading & Pressure Relief
We use padding, orthotic modifications, and footwear adjustments to reduce pressure on vulnerable areas and prevent ulcer recurrence.
Infection Prevention & Monitoring
Regular checks help detect early signs of infection before they become serious.
Footwear Guidance
Protective, properly fitted shoes reduce friction and pressure points that can lead to ulcers.
Education & Self‑Care Strategies
We teach patients how to monitor their feet daily and recognize early warning signs.
Prevention Strategies
-
Inspect feet daily for cuts, blisters, redness, or swelling.
-
Keep skin clean and dry.
-
Never walk barefoot.
-
Wear cushioned, well‑fitted footwear.
-
Seek care immediately for any new wound or skin change.
When to Seek Immediate Care
Book an urgent assessment if you notice:
-
A new wound, blister, or ulcer
-
Redness, warmth, or swelling
-
Drainage or signs of infection
-
Sudden changes in sensation
-
Pain in the foot or lower leg
Diabetic Foot Treatment in Whitby
We provide comprehensive diabetic foot care, including wound management, pressure offloading, footwear guidance, and preventative monitoring. Early treatment helps prevent ulcers, infections, and amputations, supporting long‑term mobility and safety.
Book an Appointment
If you have diabetes, regular foot assessments can prevent serious complications.
Book an appointment for diabetic foot care in Whitby
